Part 2: Tackling the obesity crisis without drugs
Part 2 of this series explores how a focus on food policy could tackle the obesity crisis.
“America has the highest chronic disease burden in the world,” lamented Robert F Kennedy Jr during a speech in April this year, prompting him to make a bold promise to the American people.
“If I have not significantly dropped the level of chronic disease in our children by the end of my first term, I do not want you to re-elect me,” said Kennedy.
Upon hearing the announcement, Calley Means, a former consultant for food and pharma companies was encouraged.
“I cannot understand why every candidate for President is not making that statement,” says Means, who now is the cofounder of Truemed and wants to incentivise healthy food habits.
“It's obviously the most important issue – 40% of high school seniors qualify as having a mental health disorder, 33% of people are pre-diabetic, 50% are overweight or obese. Life expectancy is going down. There's a systemic problem here,” he adds.
But what would it take to reduce the burden of chronic disease? Calley Means thinks “it could be fixed very easily.”
“America spends trillions of dollars a year on health care and our health is only getting worse,” says Means.
This year, the World Obesity Federation predicted that the global economic impact of overweight and obesity will reach $US4.32 trillion annually by 2035 if prevention and treatment measures do not improve.
“Nobody's asking why heart disease is going up as we prescribe more drugs for heart disease. Nobody's asking why diabetes rates are going up as we prescribe more and spend more on diabetes medications. Nobody's asking why we're spending $250 billion on cancer, but cancer rates are going up,” he says.
Means blames the siloing of medical problems as one of the biggest failures in modern medicine.
“If you have depression, diabetes, heart disease, high blood pressure, obesity, you're seeing many different doctors and taking five different medications – 80% of deaths in the developed world are tied to chronic lifestyle conditions and poor metabolic health,” he says.
The “drug first policy” in many western countries fails to solve the root cause of chronic diseases like obesity and diabetes – which are largely driven by poor food choices.
Means says, “From day one, doctors are conditioned in medical school to believe that drugs and surgery are the fix. Doctors don’t get trained to understand that food is medicine.”
It was “heartbreaking” for him to see vending machines in the corridors of Stanford Medical School, allowing these places of learning to be branding opportunities for the junk food industry. Means posted a photo on X commenting, “What are these students learning?”
A systematic analysis for the Global Burden of Disease Study 2010 found that poor diet generated more deaths and disability than tobacco, alcohol and physical inactivity combined.
Means thinks doctors might be paying “lip service” to food and lifestyle changes, but on the ground, the medical profession resorts to pharmaceutical interventions and points to the covid pandemic as an example.
“Obesity, heart disease, and diabetes were the biggest risk factors after age for poor covid outcomes. But Fauci never talked about a national plan devoted to understanding how poor metabolic health was crippling people who caught covid,” says Means.
“Instead, we spent trillions on lockdown policies, drugs, and vaccines as if they were the only serious science interventions to prevent poor covid outcomes. It was shameful,” he adds.
Corrupted science
In his previous career as a consultant for the food and drug industry, Means admits to using “evil” tactics to influence public messaging for the benefit of corporations.
“I consulted for Coke to ensure that sugar taxes failed, and that soda was included in food stamp funding in the US,” says Means.
The “first step in the playbook” he explains, was to pay millions of dollars to the civil rights organisation – the National Association for the Advancement of Colored People - to call opponents of food companies “racist.”
Means also helped Coca-Cola fund medical groups like the American Diabetes Association to create a standard of care for diabetes management, and to say that eating sugar was not a problem.
One study published in the American Journal of Preventive Medicine found that 96 national health organisations accepted money from Coca-Cola, PepsiCo or both companies between 2011 and 2015.
And in 2015, the NYTimes reported that Coca-Cola funded an organization called the Global Energy Balance Network that shifted public health messaging away from diet and onto exercise.
In fact, a seminal report by Oxfam showed that globally, the majority of processed food is produced by one of only ten huge multinational corporations: Associated British Foods (ABF), Coca-Cola, Danone, General Mills, Kellogg, Mars, Mondelez International (previously Kraft), Nestle, PepsiCo and Unilever.
“Part of the corruption is that studies are paid for, and they get scientists to author papers to say that obesity isn't caused by what you eat, but by genetics…who is going to doubt a credentialed Harvard doctor?” says Means.
He adds, “Food companies are the lifeblood of nutrition research at places like Oxford, Harvard, and Stanford. So that's why it’s rigged. These companies know how to infiltrate our trusted research and medical institutions – it’s an orgy of corruption.”
‘Toxic’ foods
Means said we need to incentivise healthy behaviours and remove toxic junk food from the environment if we are really going to move the needle.
“Ultra-processed foods make up most of the diet in the developed world. They contain three ingredients - processed added sugar, highly processed grains, and seed oils,” explains Means. “These foods have no nutrition in them, they don’t rot and its why these foods can stay on the shelf for years.”
The potential health effect of food processing and food formulation is now being widely researched, with higher consumption of ultra-processed foods linked to poorer cardiometabolic health, weight gain, and cognitive decline among other conditions.
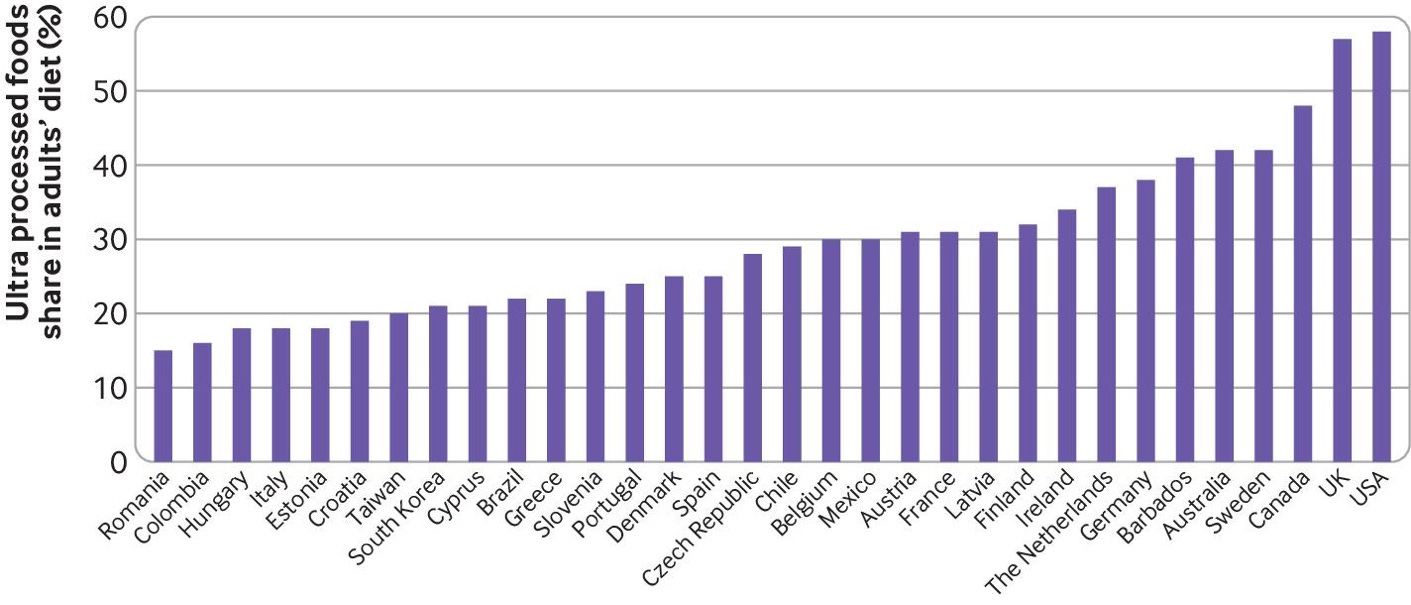
Consumption of ultra-processed foods has been increasing since the 1990s in most countries (mainly in low and middle income countries). Now, the US, UK and Canada have the highest dietary intake of ultra-processed foods.
It has only been exacerbated by the push to consume “fake-meat” alternatives which are ultra-processed, containing genetically modified components with over 20 total ingredients including protein isolates mechanically extracted from whole soy and peas, and fats which are industrial vegetable and seed oils.
A better model?
After travelling to Nordic countries like Denmark where childhood obesity is three times lower than in the US, Means says that American’s should take a leaf out of their book.
“Denmark has a program where if you earn a lower income, you get a food card and you're incentivised to buy whole food. But in the US, if you’re on a lower income, you get a card called a food stamp, and you can buy Coke. In fact, 10% of all that money goes towards Coke and sugary drinks, 70% goes towards ultra-processed food,” says Means.
“Instead, the US government subsidises drugs like Ozempic to the tune of $10,000 per patient per year and it’s the reason why people are doing cartwheels on Wall Street right now - because obesity drugs are the largest target market. Much of that money should be invested in regenerative agriculture and better food, particularly for lower income kids,” he adds.
See PART 1: Weighing up the value of weight loss drugs
Original version published at Broken Science Initiative






It's a terrible thing that you with you with your purity and clearness of thought have to cry in the wilderness about something as fundamental as eating properly.
You should have a bigger forum to reach more like-minded people.
Regards
JK
I agree with Means' diagnosis of the problem and also the solution. However, as much as I would like to believe it, I don't believe his statement that "“it could be fixed very easily.” Really? Did he not pay attention to how people reacted during Covid? "YOU CAN'T TELL ME WHAT TO DO!" Did he not notice people's anger at the proposed tax on sugar laden sodas in NY, no doubt egged on by industry executives like his former self when he worked for Coke? IMHO, it will be extremely difficult to bring about the changes he proposes, at least here in the U.S., where we prize individual freedom above all, including the freedom to kill ourselves. That sounds harsh, and I realize many people are addicted to junk food and drinks, which fuels their angst, as it's really hard to give up one's addiction, especially without professional help, which is not covered by insurance when it comes to food addiction. Perhaps Mr. Means could accomplish more good if he explained how he went from being evil to promulgating good, so we can figure out how to convince all the Big Food Executives (and the politicians they support) to give up their sins and move to the light.